I am going to give a short introduction to ROC (Receiver Operating Characteristic) curves. This term is frequently used in radiology research and I just wanted to give you a little information to know whether or not the ROC curve is significant or not.
What is an ROC curve?
An ROC curve is a way to evaluate the sensitivity versus the specificity of a test. Sensitivity is a tests ability to accurately identify a positive result. This means that when a test result is positive it accurately identifies the presence of a disease. Specificity is a tests ability to accurately identify a negative result. This means that when a test result is negative it accurately identifies the absence of a disease. These two values are charted on an x (1 – specificity or FPR in the image below) and y (sensitivity) axises. This typically results in a curved outcome on a chart.
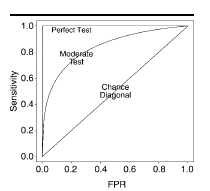 Image from Radiology – October 2003 – Obuchowski
Image from Radiology – October 2003 – Obuchowski
(she has some great articles on the topic if you are interested)
Ideal ROC curve
An ideal ROC curve is 1.0. While this is nearly impossible to achieve, a number closer to 1.0 shows a more reliable test. A ROC curve that is close to or below 0.5 is on the ‘chance diagonal’. This means that there is no statistically significance to the test being evaluated. Or in other words, the test is useless in determining the absence or presence of a disease.
Next week I will go over what research has shown for oral radiology and what the ROC curves for different imaging modalities are.
Should you have any questions or thoughts on this topic, please let me know.
Thanks and enjoy!
DR G,
This is Sharon from MCL.. Our site had a major technical issue and we are fixing that, but didnt really have a way to let you know..so i thought at least here we could send you a message.. our email is now back up, (see attached email below) as is the main pages, so please email us, so we can finish your project, even though the site isnt really fully functional quite yet.. you still wont be able to login quite yet, but we can finish via the email if we have to.. We apologize for any concern or delay
Sharon MCL
Hi again.. so sorry to keep posting here.. but the email we have is still kind of quirky, so i just found out the emails are not getting to us.. so email me personally at howarth.sharon@yahoo.com
so sorry for the inconvience.. i cant get into the database yet to get any other contact info.. I hope you are at least getting this
Sharon (MCL)